Lu, E., Solovyeva, K., Hebert, Z., Kietzer, L., Griffiths, S., Eid Antoun, Z., Keeley, T., & Alfonso-Cristancho, R., (2021, September 5-8). Shared decision making in severe asthma therapy: Qualitative study of physician-patient communication. European Respiratory Society (ERS) International Congress.
Patient engagement in biologic treatment of severe asthma becomes a driving force after first starting treatment, according to research from Verilogue and GSK, recently presented at the European Respiratory Society (ERS) International Conference 2021.
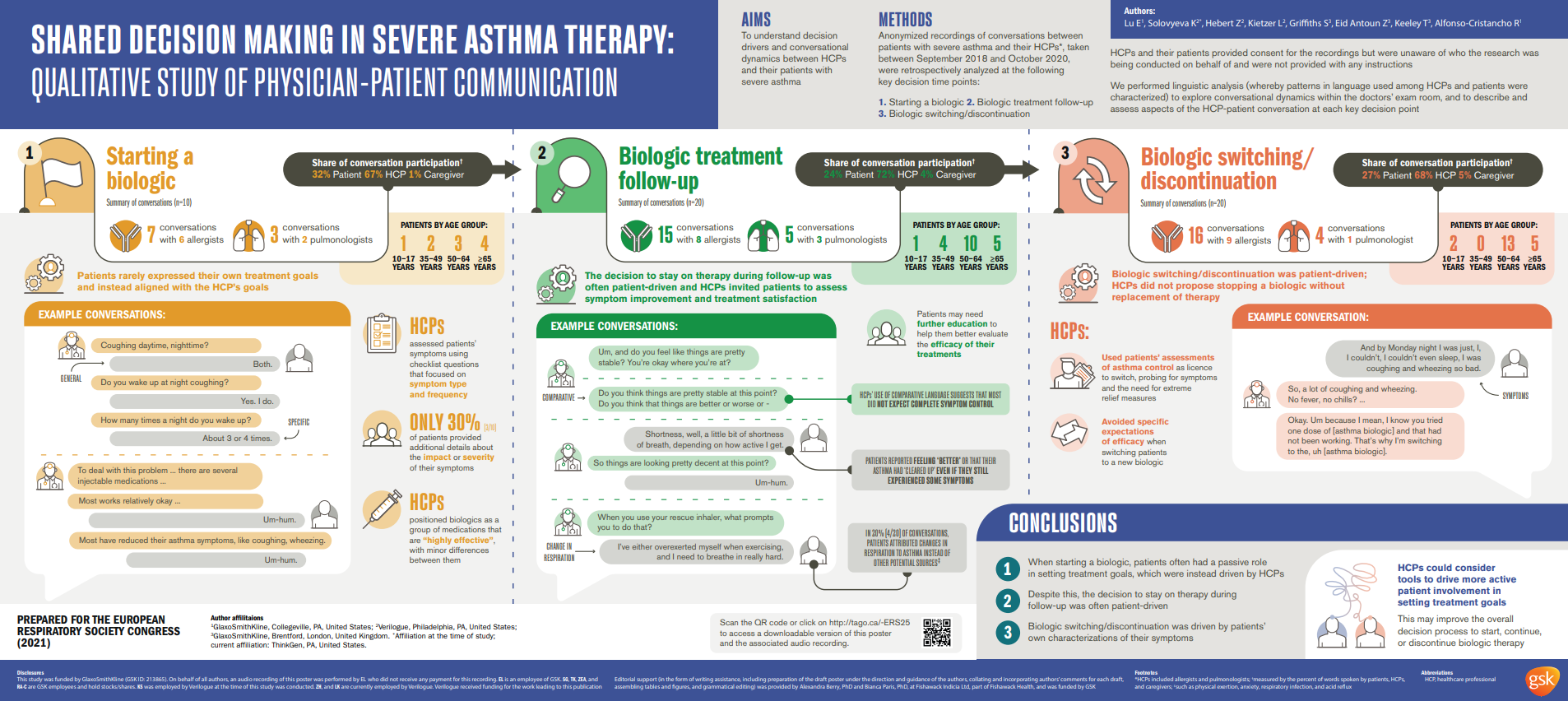
This study analyzed 50 exam room conversations between severe asthma patients and their allergist or pulmonologist. In all conversations, patients were starting, having a follow-up visit to starting, switching, or discontinuing biologic therapy for their severe asthma. Analysis focused on understanding decision drivers and conversational dynamics between HCPs and their patients with severe asthma.
The study found that although patients had a passive role in setting treatment goals when starting their first biologic, their conversational involvement at follow-up visits drove the process of deciding to either continue using their current biologic treatment or switch to another one.
-
- Patients starting a biologic rarely expressed their own treatment goals: Patients starting a biologic for severe asthma tended to have passive roles when it came to exploring and establishing treatment goals. Instead, physicians drove this part of the conversation, positioning biologics as “highly effective” and with minimal differences among different types. Patients passively signaled alignment with their physicians’ often vague treatment goals.
-
- Staying on therapy was a patient-driven decision-making process: Despite patient passivity when discussing starting a biologic for severe asthma, at follow-up, patients’ self-assessment played a key role in deciding whether to continue treatment. At follow-up visits, physicians invited their patients to self-assess symptom improvement and treatment satisfaction. This created a physician-guided, but patient-driven conversation, where patients decided to remain on biologic therapy when they experienced relative, even if not total, symptom control.
-
- Discontinuing a biologic was also patient-driven, but physicians proposed replacements: When patients’ self-assessments identified no or insufficient symptom control, physicians offered alternate biologics, rather than abandoning biologic therapy completely. When offering a replacement biologic, physicians continued to avoid setting specific expectations of the new treatment’s efficacy; however, in these contexts, they were also much less likely to use glowing descriptions that they used when patients were starting their first biologics, such as “highly effective.”
Patient self-assessment of their severe asthma symptoms after starting a biologic treatment plays an influential role in whether the patient and physician decide to stay on a current therapy or try something new, but initial goal-setting discussions lack detail from the physicians and fail to engage patients. Supporting patient participation in the first steps of biologic treatment journey can set the stage for improved conversations and decision-making down the road, when discussing continuing, switching, or discontinuing biologic therapy.
You can listen to the recorded poster presentation, presented by GSK’s Ember Lu, by clicking the button below, and to learn more about the ways that Verilogue can support your brand team, don’t hesitate to reach out to your Verilogue account representative.